

Bladder control solutions are available for the millions who experience urinary incontinence, a condition that affects daily life but is often suffered in silence. If you're searching for ways to manage bladder leaks, here are the main approaches:
Quick Overview of Bladder Control Solutions:
Urinary incontinence is not a normal part of aging, and you don't have to accept it. It's a common condition, affecting about 62% of women and 14% of men, yet many never discuss it with a healthcare provider.
Leaking urine when you sneeze, cough, laugh, or exercise doesn't have to control your life. Effective treatments exist for every type and severity of bladder control problem, from sudden urges to occasional leaks.
The first step is understanding what's causing your symptoms. Different types of incontinence—stress, urge, overflow, or mixed—respond to different treatments, which is why a proper diagnosis is so important.
As Dr. Ryan Tubre, a board-certified urologist at Rose City Urology, I've helped hundreds of patients find effective bladder control solutions custom to their specific needs. My approach combines conservative lifestyle modifications with advanced treatments like robotic-assisted procedures and nerve stimulation therapies to restore confidence and quality of life.
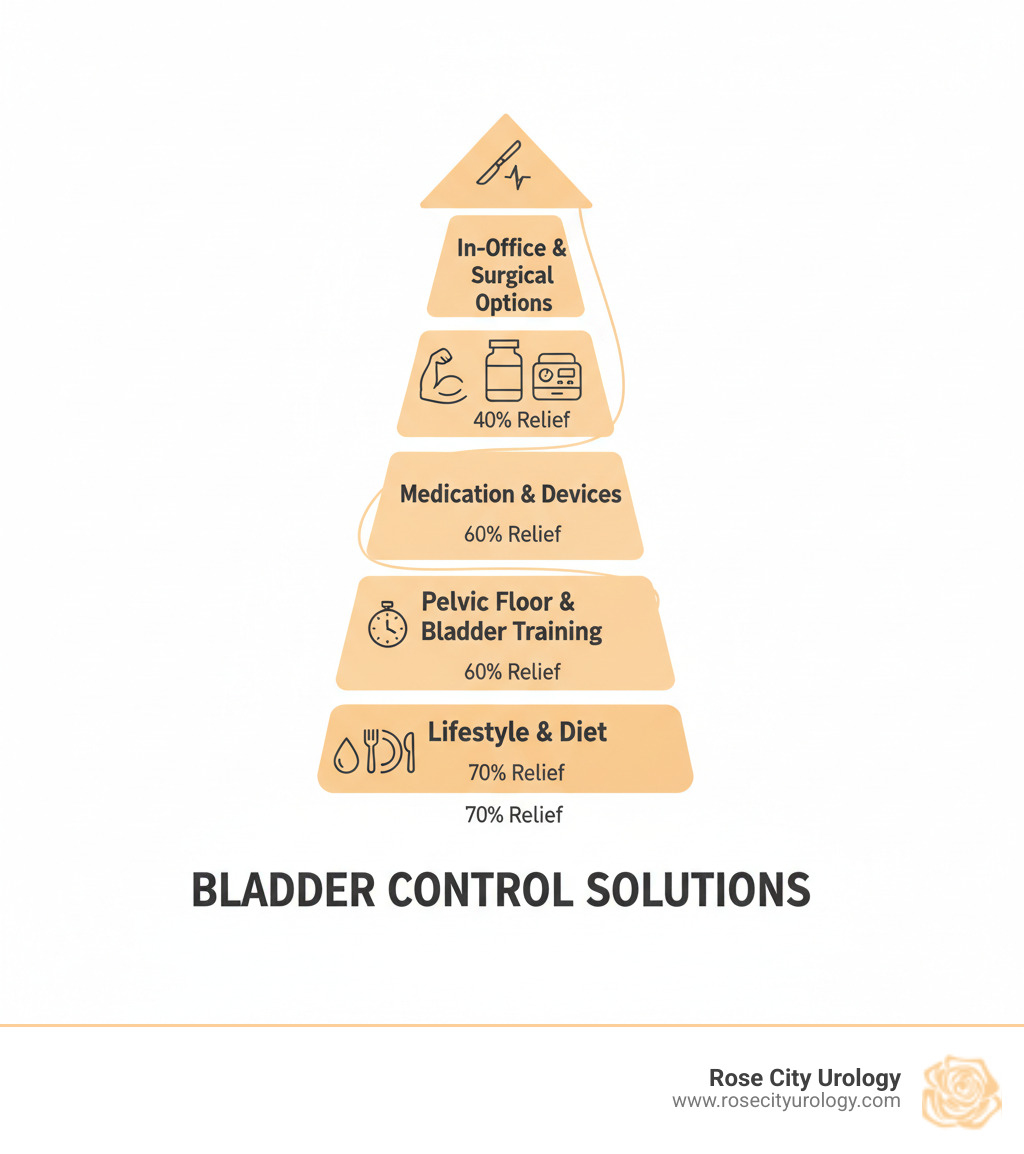
Simple Bladder control solutions word guide:
Finding effective Bladder control solutions starts with understanding what's happening. Urinary incontinence (UI) is the unintentional leakage of urine. It's not a single problem; different types have different causes. Identifying your type is the first step toward relief.
Here are the main types of urinary incontinence:
Stress Incontinence: This is leakage during activities like coughing, sneezing, laughing, or exercising, which put pressure on the bladder. It's often caused by weakened pelvic support muscles. Learn more about Stress Urinary Incontinence (SUI).
Urge Incontinence: This is a sudden, intense urge to urinate, followed by involuntary leakage. It's often called "overactive bladder" because the bladder muscles contract unexpectedly.
Overflow Incontinence: This occurs when the bladder doesn't empty completely, leading to frequent or constant dribbling of urine. It can be caused by a blockage or a weak bladder muscle.
Mixed Incontinence: This is a combination of symptoms from more than one type of incontinence, most commonly stress and urge.
The reasons for bladder leaks differ between men and women and can be influenced by other health factors.
For women, common causes include:
For men, common causes might involve:
Diagnosis starts with a detailed medical history and a physical exam. For women, this may include a pelvic exam, and for men, a digital rectal exam to assess pelvic health.
A bladder diary is one of the best diagnostic tools for finding the right Bladder control solutions.

For a few days, you'll track your habits to help us see patterns and triggers. We'll ask you to record:
This diary helps us understand your unique bladder habits and the severity of your leaks, pointing us toward the correct UI type and a personalized treatment plan. For more insights, see our page on Urinary Leakage & Incontinence.
Many other factors can worsen bladder leaks. Knowing these helps fine-tune your Bladder control solutions.
Chronic Cough: A persistent cough from smoking, asthma, or allergies constantly pressures the pelvic floor. Quitting smoking is a huge step for bladder health. Find help to stop smoking.
Constipation: Straining during bowel movements weakens pelvic floor muscles. Maintaining regular bowel habits is crucial for bladder health.
Obesity: Extra weight increases pressure on the bladder. Even modest weight loss can significantly reduce leaks.
Nerve Damage: Conditions like diabetes or injuries can disrupt signals between the brain and bladder, affecting control.
Neurological Conditions: Diseases like Multiple Sclerosis (MS) and Parkinson's can interfere with brain signals that control the bladder, causing strong urges.
Urinary Tract Infections (UTIs): UTIs irritate the bladder, causing urgency and leaks. These symptoms usually resolve once the infection is treated. Learn more about managing Urinary Tract Infections (UTIs).
Some of the most effective bladder control solutions are simple lifestyle changes. Many patients see significant improvement just by adjusting daily habits, which can be an empowering way to take control.
Living with UI can affect your confidence and social life. You're not alone. Open conversations with your provider or support groups are a powerful first step toward getting your life back. Urinary incontinence is common and treatable.
Small changes in your daily routine can lead to big improvements in bladder control.

Diet and fluid management is surprisingly powerful. What you eat and drink directly affects your bladder. The goal is smart fluid management, not dehydration. Common bladder irritants like caffeine, alcohol, spicy foods, and citrus can trigger urgency. Try cutting back to see what affects you. Don't stop drinking water, as concentrated urine is also a bladder irritant. We'll help you find the right balance to stay hydrated while managing symptoms.
Maintaining a healthy weight is a game-changer. Every extra pound adds pressure to your bladder. Research shows that even modest weight loss can bring noticeable relief from leaks.
If you smoke, quitting is one of the best things you can do for your bladder. Smoking doubles the risk for pelvic floor disorders, and a chronic smoker's cough constantly stresses these muscles. Resources like Smokefree.gov can help.
Managing constipation is also important. Straining during bowel movements weakens pelvic floor muscles. A diet with enough fiber and fluids supports both bowel and bladder health.
Common bladder irritants to watch for:
Beyond diet, you can retrain your bladder and strengthen its supporting muscles. These techniques are powerful bladder control solutions that put you in control.
Pelvic floor muscle training (or Kegel exercises) strengthens the "hammock" of muscles supporting your bladder. Stronger muscles prevent leaks, especially during activities like coughing or laughing. To do a Kegel, squeeze the muscles you'd use to stop urination. Hold for a few seconds, then relax. Aim for at least 8 contractions, 3 times daily. Consistency is key for lasting results. Proper technique is crucial; a physical therapist can help, sometimes using biofeedback to ensure you're targeting the right muscles. For more guidance, see our guide on Bladder Control Exercises.
Bladder training teaches your bladder to hold more urine. With timed voiding, you urinate on a fixed schedule (e.g., every 2 hours), gradually increasing the time between voids. Urge suppression techniques, like deep breathing or a quick Kegel, help you manage sudden urges and regain control. Bladder training programs typically last at least 6 weeks and work well with a bladder diary to track progress. For more strategies, visit our resource on Urinary Urgency Relief.
When lifestyle changes aren't enough, medical and non-surgical bladder control solutions are the next step. A consultation with a specialist at Rose City Urology is valuable for creating a personalized plan based on your specific type of incontinence and health goals.
Medications are effective for managing urge incontinence (overactive bladder) by calming the bladder muscle. We'll discuss the benefits and potential side effects to find the right fit for you.
Common side effects, especially with anticholinergics, include dry mouth and constipation. We monitor patients closely to manage these effects.
A range of devices and in-office procedures offer effective solutions, especially for stress incontinence or when medications aren't suitable.
Pessary for Stress Incontinence: A small, removable silicone device inserted into the vagina to support the urethra and prevent leaks during activities like coughing or exercising. A healthcare professional fits it, making it a great non-surgical option.
Urethral Inserts: These are small, disposable plugs inserted into the urethra to block urine flow during specific activities, like exercise.
Over-the-Counter Products: Absorbent pads, protective underwear, and specialized skin care products can help manage symptoms and improve quality of life.
Botox Injections: For severe urge incontinence unresponsive to other treatments, Botox is injected into the bladder muscle to relax it, increasing capacity. The effects last about six to nine months. Learn more on our page about Bladder Botox.
Nerve Stimulation: This treatment uses mild electrical pulses to restore proper nerve communication between the brain and bladder.
If conservative treatments don't provide enough relief, it may be time to discuss advanced and surgical bladder control solutions. For certain types of incontinence, especially stress incontinence, surgical treatments have very high success rates.
Before any procedure, we'll have an in-depth discussion about the benefits, risks, and recovery to ensure you feel confident and informed. This is a partnership decision, and we want you to feel comfortable every step of the way.
The right surgical option depends on your type of incontinence, its severity, and your overall health.
Sling procedures are the most common surgery for stress incontinence in women. A "sling" of synthetic mesh or your body's own tissue is placed under the urethra to provide support, preventing leaks during activities like coughing or laughing. The midurethral sling is a popular minimally invasive option with a quick recovery. The FDA provides detailed information on synthetic mesh used in these procedures.
Bladder neck suspension uses stitches to lift and support the bladder neck and urethra, returning them to their proper position. Though more invasive than a sling, it's an excellent option for certain patients.
An artificial urinary sphincter is a life-changing option for men with severe stress incontinence, often after prostate surgery. A small, inflatable cuff is placed around the urethra; the patient manually deflates it to urinate. It offers excellent control for those who need it.
Urethral bulking agents are a less invasive option where a substance is injected into urethral tissue to help it close more tightly. The procedure is quick with minimal downtime, but effects may diminish over time, requiring repeat injections.
Recovery varies by procedure. Minimally invasive options like slings often allow a return to light activities in a week or two. We provide detailed post-operative instructions and support you throughout your recovery, because your comfort and confidence are our priority.
It's natural to have questions when exploring bladder control solutions. Here are answers to some common concerns.
Consistency is key with Kegels. While some notice improvements in a few weeks, it typically takes 3 to 6 months of regular practice to see a significant difference. The timeframe varies based on your initial muscle strength and diligence. Proper technique is vital; ask a physical therapist for guidance if you're unsure. Research shows consistent, correct training benefits everyone with urinary incontinence.
Whether UI can be "cured permanently" depends on its cause and type. If UI is from a temporary factor like a UTI or medication, treating the cause often leads to a complete resolution. For UI from chronic conditions like weakened muscles or nerve damage, a "cure" may mean long-term management. Many effective bladder control solutions can provide significant relief, helping you achieve continence and a high quality of life.
It is generally not recommended to severely limit water intake. This can make your urine more concentrated, which can irritate your bladder and worsen urgency and frequency. The key is balance. Drink enough to stay hydrated (your urine should be pale yellow). You can be mindful of when you drink, such as limiting fluids before bed, and avoid bladder irritants like caffeine. Always talk with your healthcare provider to find the right balance for you.
If you've been struggling with bladder leaks, know this: you're not alone, and you don't have to accept this as your new normal.
We've explored a comprehensive range of bladder control solutions, from lifestyle changes to surgery. This variety means there is an effective approach for nearly every situation.
However, none of these solutions can help without a professional diagnosis. Understanding your specific type of incontinence is essential for creating a personalized treatment plan that works for you.
At Rose City Urology in Tyler, Texas, we've dedicated our practice to helping men and women reclaim their confidence and quality of life. Whether you're experiencing occasional leaks or more persistent symptoms, we're here to listen without judgment and create a treatment strategy that fits your life.
Our approach starts with the most conservative options and progresses to more advanced treatments only when needed. We use cutting-edge technology, including robotic-assisted procedures and nerve stimulation therapies, all delivered in a supportive, patient-centered environment where your comfort and dignity come first.
You don't have to organize your life around finding the nearest bathroom or avoid activities you love. You don't have to suffer in silence.
Take that first step today. Find comprehensive care for urinary leakage and incontinence at Rose City Urology, and let's work together to help you regain control and get back to living life on your terms.